 As my husband and I watched our baby moving on the sonogram screen before us, hearing the familiar fluttering that filled the darkened room, we found it nearly impossible to digest what the specialist had just told us. “I advise that you terminate this pregnancy.”
As my husband and I watched our baby moving on the sonogram screen before us, hearing the familiar fluttering that filled the darkened room, we found it nearly impossible to digest what the specialist had just told us. “I advise that you terminate this pregnancy.”
This is my PPROM story and what every woman of child-bearing years needs to know about it.
What is PPROM?
Preterm Premature Rupture of Membranes (PPROM) occurs when the amniotic sac breaks way too early (technically before 37 weeks). Mine broke just before 14 weeks. Yes, you read that correctly. 14 weeks.
Actually, I didn’t even know my water had broken. It wasn’t a huge gush of fluid like you experience with full-term pregnancies; the only symptom I had was faint spotting which led to immediate fears of a miscarriage. So when my husband I went to my OBGYN the next day, I was elated when he told me there was a heartbeat. But what he said next changed my world forever:
“But there’s no amniotic fluid.”
My sweet doctor was very calm, assuring me it was nothing I did to cause this (PPROM happens in about 4% of pregnancies). He advised me to go home, get in the bed for a week because in some rare cases the amniotic sac will reseal on its own. I didn’t have the heart to ask him what happened if it didn’t…

The Standard Medical Response
Fast forward a week and we found ourselves at the maternal-fetal specialist’s office. Our hopeful spirits were crushed when she told us that the sac did not reseal. And the spotting I had experienced was because my placenta had abrupted (probably from the force of the amniotic sac breaking, although they couldn’t say for sure).
She then proceeded to explain to us that just like when your water breaks at full-term you are told to go to the hospital because the risk of infection is high. Well, that same risk of infection is present when your water breaks too early. The amniotic sac is what protects the baby from bacteria and infection. As soon as it is breached it is not a matter of if an infection will come, but when. And when it does, the infection quickly spreads to the mother, who if not treated quick enough, could die.
Besides, the doctor told us, amniotic fluid is what develops a baby’s lung tissue. Even if by some miracle this baby made it to viability (23-24 weeks) without getting an infection, she told us, there would no way the baby could breathe upon birth. She would suffer and suffocate within a few minutes after birth.
And if by some miracle of miracles the baby didn’t die upon birth, she would be horribly disabled (amniotic fluid also allows babies to kick and move and develop muscle tissue) and hooked up to a ventilator, and probably be brain damaged (due to the placental abruption not allowing blood to flow properly to the baby) the rest of her life.
There is nothing to prepare you as expectant parents for this kind of news. But seeing the baby on the screen, hearing the heartbeat pumping away, I could not do as they advised. The specialist and her partner did not agree with our decision not to terminate. But they hesitantly said I could go home, get in the bed, and wait to miscarry or get an infection as long as I agreed to take my temperature several times daily. If I started showing signs of a fever they would absolutely have to deliver the baby because that meant certain morbidity for an under 24 week old fetus and it would only a matter of time before I succumbed, too.
“Pray for a miracle,” one of the doctors said as we walked out, my husband having to hold me up as the weight of the news was almost too much to bear.
A Glimmer of Hope
In our modern age, there seems to be few conditions or diseases without some sort of treatment, medicine, or medical trial. But that’s the case with PPROM, as our friends and family soon learned when they started researching where else we could go in the country or what else we could do to help this baby. Many things have been tried over the past few decades – patches and injecting of synthetic fluid, just to name a few. But all have been proven to actually increase infection rates so are rarely used anymore.
But then I came across a small glimmer of hope.
I found an international PPROM message board (that’s now a private Facebook group). Some of the women were on bed rest, told that their baby wouldn’t survive; others had recently terminated their pregnancies upon the advice of their doctors and were seeking support and answers after their devastating losses.
And then there were a few women on the board whose PPROM babies had survived. Granted, their water didn’t break as early as 14 weeks like my case. But the mother who said her water broke at 18 weeks and posted pictures of her then healthy two-year-old gave me the little hope I needed to get through each day. That and my faith in God, who I believed wasn’t limited by doctors’ predictions or harmful bacteria or my compromised womb.

Bed Rest
So on bedrest I stayed. I made it through the first week, then the second. I held my breath every time the doctor put the sonogram wand on my growing belly. I was just as shocked as the doctor when we heard that familiar, fast beating.
In total, I spent 15 weeks on strict bed rest with no measurable amounts of amniotic fluid, the last six in the hospital on the antepartum ward. During that time I only got out of the bed to go to the bathroom and take an occasional shower.
It was by far the most difficult thing I’ve ever done in my entire life. Most women on the antepartum ward were guaranteed a baby in the end if they just followed the doctors’ orders. But that wasn’t the case for me. I was doing all the same things while being told day after day that my baby was probably going to die upon birth . . .
But I did not give up hoping and praying and checking that message board every day for more stories of survival, stories of PPROM babies defying doctors’ expectations.
The Birth
I finally went into labor at 29 weeks, 15 weeks after my water broke, most likely due to an infection. It was an emergency situation as I had been told it probably would be. My placenta – which has been 50% abrupted the entire pregnancy – tore off completely. The pain is something I will never get over. Nor will the way my mom looked at me as they rushed me back into the ER. I seriously don’t think she knew if she would see me or her grandchild alive again that day.
But I had a peace that surpasses understanding about me. I wanted to meet the baby that I had bonded with in those otherwise lonely 15 weeks of bed rest. Even if it was only for a few minutes…
The Baby
In my foggy state, I saw the team of doctors pull the baby out of me and take her to a little room off the side of the OR. The next thing I remember they were wheeling her out of the room, at least five nurses and doctors hovering above and around her, pumping this and administering that.
They didn’t stop to let me see her and I was relieved. Why? That little incubator on wheels whizzing out of the room meant they were going to do at least try to work on her in the NICU, instead of putting her on my chest to die.
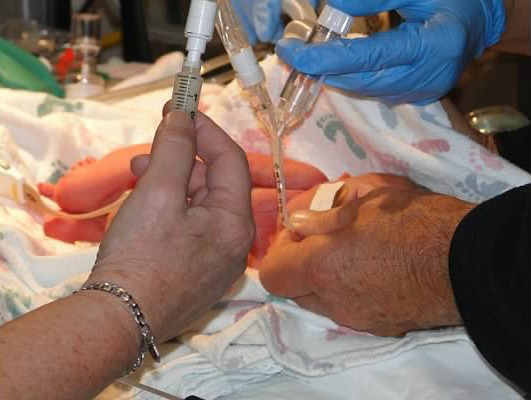
The NICU
The first few hours and days in the NICU were touch and go. At one point, the NICU doctor told my husband we needed to say our goodbyes. But our daughter kept defying odds, hanging on. They put her on a high oscillating ventilator, gave her as many steroid shots as she could take, and everything else they could possibly do to get her lungs to function.
And, you know what, they eventually did. To the surprise of every doctor and nurse.
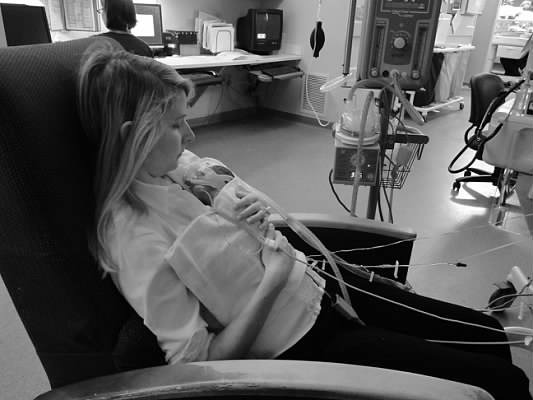
Our daughter spent a total of 2 and a half months in the NICU, which is a very little amount of time considering her story. She came home on supplemental oxygen, has had several surgeries , a feeding tube, and years of therapy for physical issues related to my pregnancy. But today she is a happy, vibrant, and joyful six-year-old, going to a rigorous academic school and defying everything doctors told us what happened to her. It’s nothing short of a miracle. But it’s also a story of hope for other moms experiencing PPROM.
PPROM Awareness
It’s mystifying to me every woman who joins this PPROM Facebook group is told by her doctor pretty much the same thing: there is no hope for their babies and they should terminate immediately because their life is at risk. But what is there is a little hope? Should that change how PPROm pregnancies are treated?
Now I realize my daughter’s story of survival after a PPROM at 14 weeks is rare, especially considering the placental abruption. But since she was born I have read more and more stories from mothers whose water broke at 16, 18, 19, 22 weeks who went on to deliver healthy – albeit premature – babies. Even women who PRROM at 24-26 weeks are sometimes told to terminate, which is crazy to me because there are plenty of former preemie babies I know who were born that early and are living normal, healthy lives today.
It’s obvious that medical journals have not captured these stories quite yet. Below I’ve listed the organizations trying to fund research and educate medical professionals about these PPROM success stories, but awareness is slow. So I humbly ask you to share this with
So I humbly ask you to share this with post with your friends. Maybe there is a pregnant mom out there who has just received the most devastating news, and she is scrolling through google search results for any glimmer of hope or support. Or maybe your have a friend that is an OBGYN or antepartum nurse who might not know that there are PPROM are stories of survival. I would love for our story to be that glimmer of hope and perhaps get the medical community to relook at its standard response to this medical condition.

Little Heartbeats Facebook Group
American Alliance for PPROM Support
BabyCenter PPROM Message Board












I’m so glad I found your story today. Just this morning, I was told that my membranes have ruptured and there is no amniotic fluid in the sac, but my baby boy still has a heart beat. I am 14 weeks 3 days so our chances of this lasting are very slim. I am struggling if I can terminate this pregnancy, but your story gives me hope. Please pray for us. I will do whatever it takes to help my baby boy.
Dear Jamie i real like to know the status your baby. I am in the same boat since Friday last week
Lee,
Thank you so much for sharing your story. It really does give me hope for my situation. This is our first baby and I just ruptured at 13 weeks and 1 day last week Thursday early am around 2am. I was confused as to what happened and didn’t think it had been my water breaking. I called my OB early the next morning and he had me come in to do an ultrasound. The tech told me I had low fluid but my baby boy still had a strong heart beat. The next day I got a call from the nurse stating to come in for another ultrasound. I went to have it done and received a phone call later on that afternoon to come in for the results. The doctor on call saw me and told me that my fluids had dropped from 3.7 to 3.6 and that there was nothing they can do for me just to go home and wait. The next day I decided to go to the ER to see if at least they can give me an IV to help me hydrate. When the results came in for another ultrasound the doctor told me that I had no measurable fluid and that in my case they are sure I will have a miscarriage. I asked if they could give me an IV to at least try since the baby has a strong heart beat and he said no that there was nothing they could do for me just to go home and wait. The doctor at the ER even told me that if it wasn’t a Catholic hospital that they would just do a d & c on me. I went home that day so devasted but my husband and I are not going to give up on our little boy. I have put myself on full bed rest and drinking lots of fluids to try and hold my baby boy in as long as possible. I have a doctors appointment today hoping he can give me some hope. Since on bed rest I have been looking for inspirational stories to help me through this. I am praying for a miracle.
Can i please kno how your pregnancy turned out and how your baby is doing my prayers are with you all
I have been on bed rest since my 8th week of pregnancy. I found out I was pregnant at just 6 weeks. The day after Valentine’s day, this baby is our little miracle. Yesterday, my water ended up breaking at 14 weeks 5 days. Not knowing what was going on or that it had happened I was taken to the ER to just get an update on my baby, all I needed them to tell me was the baby was strong and still had a heartbeat. They proceeded to tell me my water broke and with that my baby wasn’t bound to make it. Broke me apart, this is my first pregnancy. So I’m scared beyond belief, but since the moment I found out something was wrong, I have not blamed God once. He is my doctor whom I trust. I was discharged this morning, was told to come home and wait for baby to pass. I have to believe my baby has a greater chance than given. My baby has been a fighter since day one and being a high risk pregnancy, I found the baby to be stronger than me at times. I’m 14 weeks 6 days now, I will hold onto this baby of mine as long a God allows me too. I have no disbelief in miracles. All we can do is trust him through this process and not lose our bond with our babies. They give us the strength to fight for them. And as long as my baby has a heartbeat, I will fight to hold on, fluid or no fluid. Its a scary situation playing the waiting game, but I have to carry on. These are our babies, they depend on us. Thank you Lee for your story, you gave me just that small nudge I needed to keep holding onto my faith.
Experiencing same here now.and its 2020. Hope this room still exist up to now.
I’m 14 weeks and 2 days my water broke this morning,I’m in a state, the baby has no fluid,I’ve seen 3 doctors and all of them are telling me the same thing, “Terminate “but my boy is fighting,his heard beat is so strong,please keep us in prayer.
What was your outcome I am on bed rest as I type
Hi! There is hope. My water broke at 13 weeks and 5 days. I was pregnant with twins. Went on bed rest almost immediately, was told by well respected OB-Gyn that there was nothing we could do to save the babies – I got a second opinion. Went to a specialist. I leaked massive amounts of fluid from baby B almost every day (terrifying) and was admitted to hospital the day they turned 24 weeks. I was in hospital – had a scare at 25 1/2 weeks with baby b when they couldn’t find heartbeat. But on the way down for emergency csection delivery he bounced back! I thank my baby A’s intact amniotic sac for sparing us infection for so long. I delivered 2 baby boys at 31 weeks and 5 days! 4 lbs each. Baby b struggled on ventilator, steroids, oxygen levels low etc. for about 5 weeks or so. Both in Nicu for 7 (A) and 8 (b) weeks respectively. Miracles my perfectly healthy, perfectly active boys are 9 years old. They are miracles to be sure. Don’t give up. It is trying and out of our hands but there is hope. Just don’t let them do any inserting vaginal checks – risk of infection.
I had PPROM at 13 weeks with my son. He’s turning 8 next month. GOD IS GOOD. Miracles happen. I would have loved positive outcome stories when I went thru this. I was also told to terminate, but refused. Follow your maternal instincts and have faith! I was told the same thing about wheelchairs, deformities, oxygen etc. The twins are going to third grade and are healthy and thriving. With the exception of being on the smaller side, they’re doing amazing! Hang in there mamas!
My water has broke at 15 weeks and I found out at my 20 week anatomy scan. This story has gave me so so so much hope.
Wow! I felt like I was reading my own story. Ruptured at 17 weeks, found a glimmer of hope in the Facebook groups you mentioned, and carried out son to 31+3. I spent 40ish days on bedrest at home and 60 days in the hospital. Our miracle baby spent 32 days in NICU. He is almost 2 and has no special needs. God is good #believe